|
Nonetheless, acuity of presentation and gravity of clinical picture dictates course of care and necessity of preoperative imaging. Other diagnostic options include echocardiography (transthoracic or transesophageal) and magnetic resonance angiography (MRA). Moreover, CTA has superior spatial resolution for the characterization of dissection flaps and evaluation of luminal patency ( Figure 1). Contrast-enhanced computed tomography angiography (CTA) is often the imaging modality of choice, as it is readily available, non-invasive, reproducible, and prompt ( 8). Imaging can help direct care and gauge level of urgency, particularly if there is pericardial, mediastinal, or pleural hemorrhage. Depending on the location of the dissection, additional diagnostic cues may include neurologic deficits, visceral pain or dysfunction from malperfusion, pulse differentials, and a murmur from aortic valve insufficiency.ĭiagnostic imaging plays a pivotal role in confirmation of diagnosis and the classification and localization of intimal tears. Patients typically present with acute-onset severe chest or back pain, often described as “tearing,” that can be migratory. The incidence of aortic dissection is 3–4 cases per 100,000 patients per year according to the International Registry of Acute Aortic Dissections (IRAD), with a well-documented male predilection ( 5- 7). Other associated risk factors include smoking history, dyslipidemia, deceleration trauma, certain drugs (i.e., cocaine), and connective tissue disorders ( 3, 4). Acute aortic rupture represents the most common cause of death in patients with aortic dissection ( 1).Īlthough the etiology of aortic dissection is multifactorial, hypertension is considered the most prevalent risk factor ( 2). The intramural hemorrhage, whether classical dissection or IMH, weakens the structural integrity of the aortic wall, predisposing it to both false lumen aneurysmal degeneration and rupture. If the hemorrhage remains thrombosed, the process is called intramural hematoma (IMH). 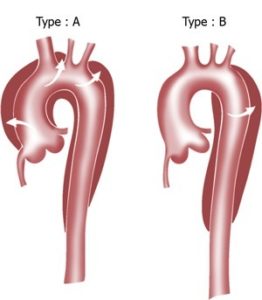
This results in the characteristic pathology of aortic dissection. If the intramedial space has both entry and exit tears, then the newly formed false lumen channel can conduct blood flow, and a membrane-like dissection flap can be observed by cross-sectional imaging. Though the precise pathophysiology is not conclusively reconciled, it is theorized that the hematoma arises spontaneously in the media and then propagates through the overlying intima to create an intimal tear, or the tear arises spontaneously or traumatically through the intima and introduces aortic blood into the intramedial space. Considered a component of the “acute aortic syndrome” spectrum, aortic dissection is characterized by propagation of a hematoma within the aortic media.
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
